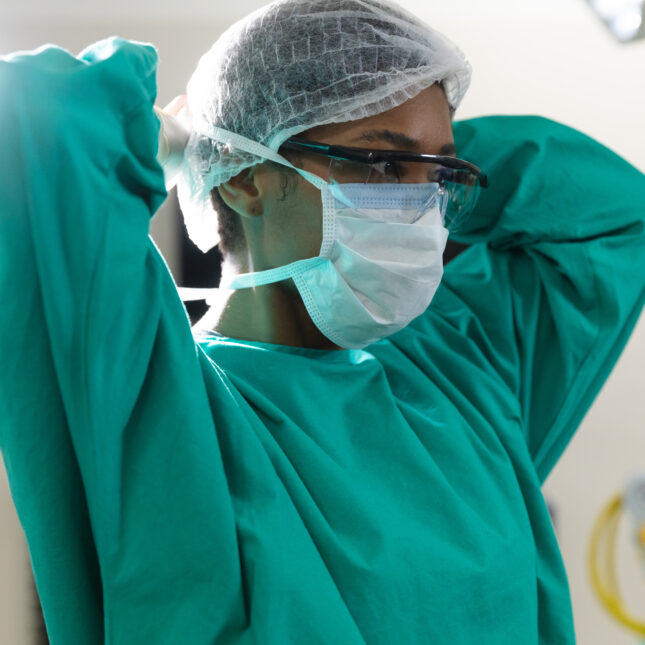
A new study published Wednesday in JAMA Surgery suggests that patients treated by female surgeons have lower rates of adverse postoperative long-term outcomes including death compared to similar patients treated by male surgeons. Long-term is defined as any outcome within 90 days or within a year.
The new study builds on previous research that had similar findings about patient outcomes related to the sex of the surgeon, but within 30 days, the traditional time period used to examine surgical outcomes, including in the National Surgical Quality Improvement Program.
“In recent years surgeons have come to appreciate that the effects of surgery can linger for longer than 30 days,” said Christopher Wallis, first author and urologic oncologist at Mount Sinai Hospital and University Health Network in Toronto. “Outcomes that are longer are much more about the thought process and the whole overall care pathway delivered to a patient. And so I think that’s why it’s important to complement 30 day outcomes with longer outcomes.”
Researchers looked at data including more than 1 million patients who underwent one out of 25 possible common elective or emergent surgeries. A total of 151,054 patients were treated by a female surgeon and 1,014,657 were treated by a male surgeon. The population-based retrospective cohort study was conducted in adults in Ontario, Canada, who had surgeries between 2007 and 2019.
Patients treated by male surgeons were 25% more likely to die within 90 days, and 24% more likely to die within a year when compared to patients treated by female surgeons. Similarly, patients treated by male surgeons were 5% more likely to be readmitted to the hospital within 90 days, and 4% more likely to be readmitted within a year. And patients were 9% more likely to experience complications within 90 days and within a year.
Even though female surgeons were a smaller subset — with 700 female surgeons being compared to 2,306 male surgeons — a difference was still seen, which paper co-author Angela Jerath found impressive. “The way the analysis is done is that even though women form a smaller subset here, the patients have been matched in a way that they look as similar as we can make them whether you’re being operated on by a male and female surgeon and you still see this difference,” said Jerath, who is a cardiac anesthesiologist at Sunnybrook Health Sciences Centre and an associate professor at University of Toronto.
Wallis clarified that while patients were not directly matched, unlike in the previous study from 2017, statistical modeling techniques are used to account for differences in patient, surgeon, anesthesiologist, procedure and hospital factors.
Researchers also found that while in general patients had better outcomes with female surgeons, female patients fared far worse than expected and had higher rates of adverse postoperative events within a year when treated by male surgeons.
What are women doing differently? It most likely has to do with what surgeons are doing outside of the operating room. By looking at specific traits that impact care, Jerath said, everyone in the health care system can benefit.
“It’s not because females are technically better surgeons,” said Cassandra Kelleher, an associate professor of surgery at Harvard Medical School and pediatric surgeon at Massachusetts General Hospital. She was not involved in the research. “It’s because somehow women are either preparing patients for surgery better, as suggested by their elective patients having better outcomes than emergent patients.”
Kelleher speculated that maybe female surgeons are also discussing what postoperative care might look like, so patients can adhere to those recommendations, or they’re listening to patients more after surgery.
“There’s something qualitatively different about the kind of practice that female surgeons have,” Kelleher said.
Prior studies have shown that there is concordance between practice style and physician-patient communication, which can affect patient outcomes for male and female physicians. “The novelty of our work is showing that these known differences in practice pattern translate to clinical outcomes for patients,” Wallis said.
“The most poignant point about this [study], I think, is their concluding statement, which is to provide the best patient care, organizations should not only support women physicians but they need to learn how women are accomplishing these better outcomes,” Kelleher said.
Women have been historically underrepresented in surgery in the U.S. — sometimes making up less than 10% in certain specialities like orthopedic and thoracic surgery. Despite making up over half of all medical student enrollments, surveys have shown that a high proportion of women residents in surgical specialties report harassment or discrimination by their male, direct supervisors as one reason for opting out. As surgeons, women are less likely to receive referrals, work on high-complexity cases, and have less operative time. They also are less likely to have leadership positions and leave academic medicine at a higher rate than men, according to Kelleher.
In the future, the researchers will look at other aspects of the patient care pathway, which includes other members of the health care team, like residents, nurses, social workers, and other support staff to see how that might affect patient outcomes.
“And then we’re working with a really skilled anthropologist to try and do some qualitative research observing surgeons as they interact with their patients and plan patient care to see if we can understand the whys behind these observations,” said Wallis, an assistant professor of surgery at the University of Toronto Medical School. He added that surgery is a “whole continuum of care beginning prior to the decision to operate and continuing long past the conclusion of the operation.”
Eventually, the research team hopes to not just know that there are differences between the way that men and women practice, but to understand why there are differences.
However, among the study’s limitations, the research team was not able to account for race and ethnicity, professional hierarchy, years of experience, training, or case complexity because of limited data. They also could not account for other team members, like nurses and residents, whose roles also have an impact on patient care.
“I think the focus should be on bringing more female surgeons into the fold, increasing the diversity within surgery as a whole, not just from a gender standpoint, but from making our surgical workforce look more like our patient population that we serve,” said Catherine Sharoky, an assistant professor of surgery at the University of Pennsylvania who also works in the division of traumatology, surgical critical care, and emergency surgery. She was also not involved with the study. “Studies like this one and ours, I think help to keep that discussion going forward.”
Sharoky’s 2018 study, aptly called “Does Surgeon Sex Matter?” looked at the difference in practice style between male and female surgeons, who had similar cases, the same amount of clinical experience at the same hospitals, and treated similar patients and found that patient outcomes were equivalent.
Kelleher agreed, adding that people who have unique perspectives and unique life experiences could bring different perspectives to caring for patients and improving outcomes.
“It’s not saying that we were doing a great job, but we could do better. Right? It’s not personal,” Kelleher said. “It’s not man versus woman. It’s not technical skill or, you know, prowess or anything. It’s just another tool to take better care of patients,” Kelleher said.










Exciting news! STAT has moved its comment section to our subscriber-only app, STAT+ Connect. Subscribe to STAT+ today to join the conversation or join us on Twitter, Facebook, LinkedIn, and Threads. Let's stay connected!
To submit a correction request, please visit our Contact Us page.